Perineal Tear during Vaginal birth
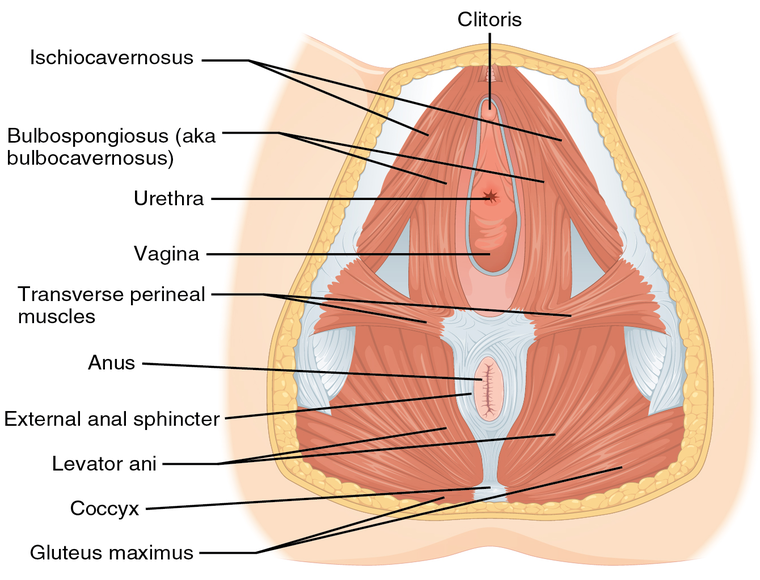
It may be stating the obvious, but a vaginal delivery requires your vagina to stretch. Everyone who delivers vaginally (and sometimes those who have a lengthy labor before delivering via C-section) can expect some perineal postpartum pain. And it’s common, given the pressure from your baby’s head pushing through, to experience tears and lacerations in your perineum (the area between your vagina and your anus) and sometimes your cervix as well during vaginal birth. As many as half of all women will have at least a small tear after childbirth.
What are vaginal tears?
Vaginal tears are common during childbirth. They occur when your baby’s head is too large for your vagina to stretch around. Women at a higher risk of vaginal tears include:
- first-time mothers
- mothers whose babies have a high birth weight
- mothers who had a long delivery
- mothers who had assisted birth, such as with forceps or vacuum
Tears can heal within 7 to 10 days with appropriate treatment. However, you can be sore for a few weeks afterward.
Depending on the severity of the tear, you may receive stitches or prescriptions for medicated creams and ointments.
Types Of Perineal Tear
According to the extent of tearing, Perineal tears are classified as:
1. First-Degree Perineal Tear:
- They are the mildest vaginal tears, and only involve the tearing of the skin around the vaginal opening or the perineal skin.
- You may experience a mild irritation or burning sensation while urinating.
- The first-degree tears usually heal within one week, and may not require any stitches.
- To overcome the pain during urination, you can take some lukewarm water in a squeezy bottle and pour it into on your vulva. The water soothes the irritation, and you can comfortably pass your urine for the first week after childbirth.
2. Second-Degree Perineal Tear:
- The tearing of the perineal muscles, which lies between your vagina and anus, imposes the second-degree vaginal tear. The perineal muscle usually supports our uterus and rectum.
- 2nd degree tears often require stitches and the damage heals within the first two to three weeks after childbirth.
- To overcome the pain of second-degree tear, you can follow some of the simple tips. You can try to sit on a pillow or a padded ring to provide additional support to your vagina.
- You can pour lukewarm water using a squeeze bottle over your vulva while passing your urine.
- After a bowel movement, try to clean your back portion softly, so that it does not rub against the wounded vaginal region.
- Apply ice pack to the wounded vaginal region, to overcome the severe pain and irritation. You can also place a chilled witch hazel pad in your sanitary napkin and wear it.
- Your doctor may prescribe you to intake stool softeners or pain relievers to soothe the unbearable pain of tears.
3. Third-Degree Perineal Tear:
- The tearing of the perineal muscles and the delicate muscle around your anus called the anal sphincter imposes 3rd degree tear.
- Such a perineal tear often gets treated in the operating room, and it may take months to heal.
- To overcome the severe pain, you can try to sit on a pillow or a padded ring after the delivery.
- You can pour lukewarm water on your vulva while urinating or place an ice pack on the wounded vaginal region.
4. Fourth-Degree Perineal Tear:
- It is the most severe form of vaginal tear that involves tearing of the perineal muscles, anal sphincter and the tissue lining of your rectum.
- 4th degreetear always gets treated in an operating room, and it may take several months to heal.
- Some of the common complications that can occur are painful intercourse and fecal incontinence.
- Your gynecologist may evaluate your condition at the postpartum checkup, and may refer you to visit a colorectal surgeon, urogynecologist, or some other medical specialists.
What are the risk factors for vaginal tears?
Some women are more likely than others to experience a vaginal tear. Risk factors include:
- assisted birth during delivery, such as forceps or vacuum use
- baby’s shoulder is stuck behind your pubic bone
- being of Asian descent
- induced labor
- first baby
- large baby
- older mothers
- prolonged second stage of labor
If your doctor knows you’re at risk for a vaginal tear, they may recommend perineal massage in the weeks leading up to your baby’s birth. Perineal massage can help to stretch the tissues between the vagina and anus to ideally allow the tissue to relax and let your baby pass through more easily. Your doctor or midwife may recommend starting it at about 34 weeks into your pregnancy.
The technique involves stretching the tissues of your vagina, much as you will when your baby passes through. However, you shouldn’t use this technique if you have a vaginal infection or vaginal herpes.
Taking care of your perineum
Here are a few ways you can take care of your perineum:
Keep it clean and free from infection
- Personal hygiene is very important. We recommend that you have at least one full shower and wash your perineal area three to four times each day
- Change sanitary pads at least every four to six hours to keep the wound as clean as possible
- Always pat the perineal area dry from the front to the back after washing to avoid introducing germs from the rectum into the vaginal area. It is also very important to wash the perineum after a bowel motion.
- Do not use a hair dryer to dry your perineum. This may delay healing or cause burning to the genital area.
- Antibiotics may be prescribed to help prevent wound infection and wound breakdown.
Keep comfortable
- Apply ice packs to the perineal area every couple of hours for the first 12–24 hours after birth. Your midwife will advise you on this while you are in the hospital. You may find the ice packs helpful for pain relief for a longer period (i.e. 24–48 hours)
- Take regular pain relieving medications. These will be prescribed by your doctor
- Try to only stand and sit for short periods of time as this places strain on your perineum. When feeding your baby shift your sitting position and lie down occasionally to reduce the pain
- Lie down to rest for between 20–40 minutes every hour for the first two to four days as this will help the stitches to heal
- Avoid double leg movements, “sit up” actions and lifting heavy weights (including picking up other children) as this places extra strain on your perineum
- Get in and out of bed over on your side as this reduces the strain on your perineum
Emptying your bowels
- For the first few days after repair, a low fibre diet is recommended to prevent any further damage due to straining to pass a stool. After the 3rd day, a high fibre diet is commenced. This will produce a stool which is easier to expel
- Keep the stools soft and ask for help if the bowels have not opened within 48 hours
- Try not to strain when using your bowels and use the recommended defecation position that is taught to you by the physiotherapist (see diagram included). The passage of hard stools can disrupt repair and delay healing
- Support the perineum with your hand while emptying your bowels, laughing, coughing, sneezing, etc.
- To assist with emptying of the bowel, bulking and softening agents such as Fybogel or Metamucil and Agarol or Lactulose are usually recommended for several days after repair. Make sure you drink a lot of water with these medications, because this will assist to reduce the likelihood of constipation occurring
- If you are prone to constipation, use bulking or softening agents up to six weeks after repair. Again, discuss this with your doctor first.
Exercises to help you recover
- We recommend you avoid pelvic floor strengthening exercises for six weeks after the birth of your baby. This is because exercise of this type can strain the wound and cause wound breakdown
- Your physiotherapist will teach you how to activate your muscles prior to moving. This will help protect your perineum as it heals
- Your physio will also teach you how to do gentle pelvic floor pulses, to improve circulation and decrease swelling and pain
When to call your doctor
If your perineum becomes very red, very painful and swollen, or if you detect an unpleasant odor, you may have developed an infection, so be sure to get in touch with your practitioner.
Also read – C-section vs. Normal delivery – How are they different?